Normal horse urinalysis provides critical insights that often get overlooked until something goes wrong. Whether you’re evaluating a performance horse showing subtle fatigue, investigating unexplained weight loss, or monitoring a patient recovering from colic surgery, interpreting urine results correctly makes the difference between early intervention and advanced disease.
Urinalysis in horses can be useful diagnostically but not as useful as in other species like small animal as we have less urinary issues in horses than small animals. In some cases it can help with kidney function but that often requires more comprehensive diagnostic tests more than just an urinalysis which are not typically performed in the field. I am not sure the examples you give are the best and ones were I typically think an urinalysis would be useful.
The challenge isn’t just running the tests—it’s understanding what those numbers mean for your equine patient. CompanAIn’s AI-powered lab interpretation tools help veterinarians contextualize urinalysis results alongside medical history, lab trends, and clinical findings through specialized AI agents trained on veterinary data.
Understanding Equine Urinalysis Basics
Urinalysis forms part of the minimum laboratory database for comprehensive equine health assessment. Alongside complete blood counts and serum biochemical profiles, urine analysis reveals kidney function details that blood work alone cannot provide, as noted by Cornell University College of Veterinary Medicine’s diagnostic protocols.
Urinalysis detects early kidney disease before azotemia develops. By the time creatinine and blood urea nitrogen climb above reference ranges, significant nephron damage has already occurred.
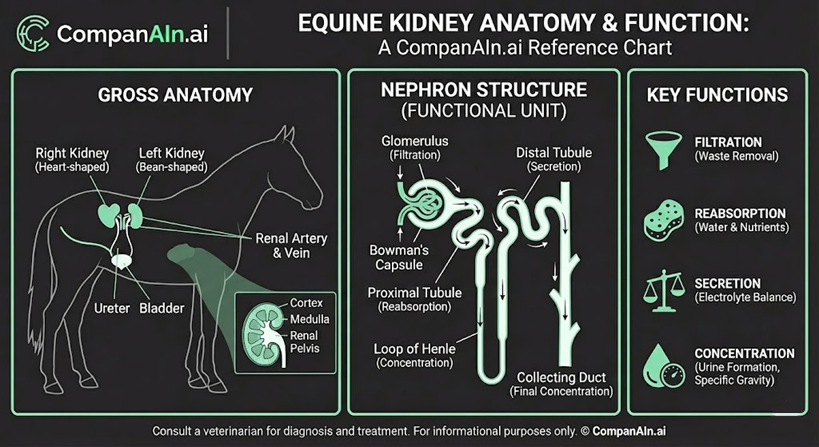
Physical Examination: What Normal Looks Like
Color and Clarity Standards
Healthy equine urine ranges from pale yellow to deep tan—similar to cider in appearance. Unlike other species, horses produce characteristically turbid urine even when perfectly healthy.
The cloudiness comes from calcium carbonate crystals and mucus, both completely normal findings in adult horses. Free-catch samples typically appear cloudier than catheterized specimens because crystals settle in the bladder and get expelled toward the end of urination. This pattern is normal equine physiology, not pathology.
Specific Gravity and Concentration
Normal equine urine specific gravity ranges from 1.025 to 1.050, with corresponding osmolality between 900 and 1,200 mOsm/kg, according to veterinary research published in clinical pathology studies. These values reflect the kidney’s remarkable concentrating ability—three to four times greater than serum osmolality. We typically consider a specific gravity of 1.020 normal so may want to adjust reference ranges.
Always measure specific gravity with a calibrated refractometer, never dipsticks. Dipstick measurements lack accuracy for equine samples and can mislead clinical decisions.
Context matters tremendously. A dehydrated horse with concentrated urine (>1.035) and elevated creatinine likely has prerenal azotemia. That same creatinine elevation with dilute urine (<1.020) suggests intrinsic renal disease.
Daily Urine Production Volume
Healthy horses produce between 5 and 15 liters of urine daily, though individual variation exists based on diet, climate, and activity level. Research from equine veterinary journals shows horses grazing lush pasture or working hard in hot weather may produce volumes at the higher end of this range.

Chemical Parameters: Beyond the Dipstick
pH Range and Alkalinity
Equine urine pH normally runs alkaline, between 7.0 and 9.0. This distinguishes horses from carnivores, whose urine tends acidic. Adult horses maintain this alkaline state consistently, while foals may show neutral pH until their digestive systems mature.
Diet influences pH significantly. Horses fed primarily concentrates show pH values closer to neutral, while those on forage-based diets maintain higher alkalinity. Vigorous exercise can temporarily shift pH toward acidic ranges as metabolic acids enter circulation.
Aciduria in horses warrants investigation. Potential causes include metabolic acidosis, prolonged anorexia, dehydration, or bacteriuria from urease-producing organisms.
Protein Detection and Interpretation
Normal equine urine contains less than 100 mg/dL protein. Alkaline urine commonly generates false-positive results on dipstick tests, making chemistry analyzer confirmation essential for accuracy.
The protein-to-creatinine ratio provides more reliable assessment than dipstick alone, as explained in VCA Animal Hospitals’ urinalysis guidelines. Ratios below 0.5:1 indicate normal protein excretion. Values exceeding 1:1 suggest pathologic proteinuria requiring further investigation.
Transient proteinuria occurs after strenuous exercise or in well-concentrated samples (specific gravity >1.030). These situations don’t necessarily indicate kidney disease. Exercise-induced proteinuria typically resolves within 24 hours, while persistent elevation suggests underlying glomerular pathology.
Glucose and Ketone Findings
Normal equine urine should not contain glucose. The renal threshold sits around 160 to 180 mg/dL—when blood glucose exceeds this level, glucose spills into urine. Persistent glycosuria indicates diabetes mellitus, often associated with pituitary pars intermedia dysfunction.
Ketones rarely appear in healthy horse urine. Their presence suggests metabolic disturbance, though they’re less clinically significant in horses than in other species.
Microscopic Sediment: Reading the Details
Normal Crystalluria Patterns
Calcium carbonate crystals dominate equine urine sediment—their abundance is expected and normal. These crystals appear more numerous toward the end of micturition as they settle in the bladder and get flushed out. Calcium phosphate crystals occasionally appear in healthy horses.
Crystal type and quantity shouldn’t raise concern unless accompanied by other abnormalities. The absence of normal crystalluria might actually warrant investigation, as clear urine can indicate inadequate concentrating ability.
Cellular Components and Casts
Red blood cells should number few to none in normal equine urine. White blood cells similarly should appear sparingly. More than 10 leukocytes per high-power field suggests infectious or inflammatory disease, warranting urine culture and additional diagnostics.
Casts indicate tubular damage, inflammation, or infection regardless of type. These protein structures form when tubular cells and Tamm-Horsfall glycoprotein aggregate within nephron tubules, as detailed in veterinary clinical pathology resources from Cornell’s eClinPath. Their presence always deserves clinical attention.
Bacterial counts in normal urine remain minimal. Catheterized samples growing more than 10,000 colony-forming units per milliliter confirm urinary tract infection.
Glomerular Filtration and Renal Function
Understanding GFR Measurements
Glomerular filtration rate in healthy horses ranges from 0.6 to 2.0 mL/kg/min, as established through veterinary renal function studies. For a 500-kilogram horse, this translates to filtering between 12,000 and 14,000 liters of plasma daily—a staggering volume highlighting the kidney’s workload.
Accurate GFR measurement requires substances that undergo glomerular filtration without tubular reabsorption or secretion.
Inulin serves as the gold standard experimentally, though iohexol clearance has become more practical clinically, as demonstrated in UC Davis Veterinary Medical Teaching Hospital’s clinical laboratory services.
GFR assessment detects early renal disease before conventional markers like creatinine become abnormal. Serum creatinine doesn’t rise until roughly 75% of nephrons lose function, making GFR the more sensitive indicator.
Advanced Function Assessment
The urine-to-serum creatinine ratio helps distinguish prerenal from renal azotemia. Ratios exceeding 50:1 indicate adequate concentrating ability, supporting prerenal causes. Lower ratios despite dehydration suggest intrinsic kidney disease.
Differentiating Normal from Abnormal Findings
Interpreting Azotemia in Context
Prerenal azotemia presents with elevated blood urea nitrogen and creatinine alongside concentrated urine (specific gravity >1.035). The kidneys function normally but receive inadequate blood flow due to dehydration, shock, or cardiac issues.
Renal azotemia shows similar blood values but with inappropriately dilute urine for the degree of dehydration present. Specific gravity below 1.020 in an azotemic, dehydrated horse strongly suggests intrinsic kidney disease. This distinction drives treatment decisions.
Collection Method Considerations
Free-catch samples during natural urination provide adequate specimens for most clinical purposes. They’re non-invasive and stress-free but risk contamination from external genitalia or environmental sources.
Catheterized samples offer cleaner specimens for bacteriology. However, the catheterization process requires sedation in many horses, and alpha-2 agonist sedatives like xylazine cause diuresis and temporary hyperglycemia that can confuse results.
Clinical Application and Integration
Combining Urinalysis with Blood Work
Urinalysis should accompany complete blood counts and serum biochemistry during initial diagnostic evaluations. Changes in renal blood parameters lack proper context without concurrent urine analysis.
This is a very good and important point to stress an urinalysis without CBC and chemistry results is not as valuable.
A horse with elevated creatinine and concentrated urine presents differently than one with elevated creatinine and dilute urine—yet the blood work looks identical. The urine makes the diagnosis clear.
CompanAIn’s platform integrates these data streams, analyzing patterns across labs, medical records, and clinical notes. The AI recognizes connections that isolated test review might miss, flagging emerging trends before they become critical. With specialized AI agents for health analysis, veterinarians receive context-aware insights that enhance clinical decision-making.
Monitoring Protocols for Serial Assessment
Establishing baseline urinalysis values for individual horses enables more meaningful interpretation when illness occurs. Serial monitoring tracks disease progression or treatment response over time. CompanAIn’s Living Memory technology stores and contextualizes past lab results, creating a comprehensive health timeline for each patient.
I agree ideally a baseline urinalysis is good to have but in the equine vet world I would say is very rarely performed. Many vets and owners will do baseline bloodwork, CBC and chem, but not urinalysis as it is not typical and it can be difficult to get a sample.
Frequency depends on the clinical situation. Horses with chronic kidney disease benefit from monthly to quarterly monitoring. Those recovering from acute kidney injury may need daily or weekly assessment initially.
Ready to Transform Equine Health Monitoring With AI?
Normal horse urinalysis interpretation should feel straightforward, informed, and actionable. Whether you’re establishing baseline values for a new patient, tracking chronic kidney disease progression, or investigating acute changes, the right analytical tools make all the difference.
CompanAIn’s multi-agent AI system analyzes urinalysis results alongside your horse’s complete medical history, identifying patterns and trends that single-test review might miss. From predictive health alerts to clinician-grade reports, our platform transforms raw lab data into proactive care strategies. Explore CompanAIn’s veterinary AI tools today and discover how intelligent health analysis supports better outcomes for every equine patient.
Frequently Asked Questions
What makes equine urinalysis different from other species?
Equine urine differs fundamentally from carnivore urine in several ways. The characteristically alkaline pH between 7.0 and 9.0, normal turbidity from calcium carbonate crystals and mucus, and higher specific gravity range distinguish horse samples. Dipstick analysis proves reliable only for pH, glucose, protein (except in alkaline samples), pigment, and bilirubin—other parameters require laboratory confirmation.
How should I interpret urine specific gravity in my patient?
Always use a calibrated refractometer for accurate measurement. Normal range spans 1.025 to 1.050. In azotemic patients, concentrated urine (>1.035) points toward prerenal causes like dehydration, while dilute urine (<1.020) despite azotemia suggests renal disease. Never interpret specific gravity in isolation—always correlate with hydration status, serum values, and clinical findings. Again we typically consider 1.020 normal
Is proteinuria always abnormal in horses?
Not necessarily. Trace protein or mild proteinuria can occur in well-concentrated samples (specific gravity >1.030) and after strenuous exercise. The protein-to-creatinine ratio provides more reliable assessment. Ratios below 0.5:1 indicate normal excretion, while values above 1:1 suggest pathologic proteinuria. False-positives occur commonly in alkaline urine, so chemistry analyzer confirmation beats dipstick results.
What does a positive occult blood test mean?
Positive occult blood indicates hematuria, hemoglobinuria, or myoglobinuria—the test cannot distinguish among these. Plasma examination differentiates intravascular hemolysis (pink plasma) from myoglobinuria (clear plasma, as myoglobin clears rapidly) from actual hematuria. Microscopic sediment examination confirms red blood cell presence, helping identify the blood source.
How significant are calcium carbonate crystals?
Calcium carbonate crystalluria is completely normal in healthy horses. These crystals create the characteristic cloudy appearance of equine urine and become more abundant toward the end of urination. Their presence reflects normal physiology and dietary calcium metabolism. Conversely, abnormally clear urine lacking expected crystals may indicate inadequate concentrating ability.
When should I be concerned about urine clarity changes?
Changes from normal turbidity to excessive cloudiness may indicate abnormal crystal accumulation, inflammatory cells, bacteria, casts, lipids, or reproductive tract contamination. However, normal variation during micturition is expected. Abnormally clear urine warrants investigation for dilution disorders or chronic kidney disease.
What is the significance of elevated leukocytes in sediment?
More than 10 leukocytes per high-power field associates with infectious or inflammatory disease. This finding warrants urine culture to identify bacterial pathogens and guide antimicrobial selection. White blood cell casts specifically indicate upper urinary tract inflammation or infection affecting the kidneys themselves.
How do I distinguish between normal and abnormal urine pH?
Normal equine urine maintains alkaline pH between 7.0 and 9.0. Aciduria is abnormal and may indicate metabolic acidosis, vigorous exercise, bacteriuria, prolonged anorexia, or dehydration. Concentrate feeding shifts pH toward neutral compared to forage-based diets. Foals naturally show more neutral pH than adults until weaning.
Should urinalysis be performed concurrently with blood work?
Absolutely. Urinalysis should accompany CBC and serum biochemistry during initial diagnostic evaluation. Renal parameter changes cannot be properly interpreted without concurrent urine results. The combination distinguishes prerenal, renal, and postrenal causes of azotemia—distinctions impossible from blood work alone.
Again I am not sure this is an accurate statement and I can say urinalysis in horses are not performed concurrently with bloodwork unless there is a concern with the kidneys or urinary system. This may not be the right answer but that is what is typically performed and again the difficulty with getting an urine sample in a horse is part of the issue.
What is the significance of casts in equine urine?
Any cast presence indicates tubular damage, inflammation, or infection. These cylindrical structures form from sloughed tubular cells and Tamm-Horsfall glycoprotein within nephron tubules. Different cast types suggest different pathologies—granular casts indicate cellular degeneration, cellular casts suggest active inflammation, and white blood cell casts strongly suggest pyelonephritis.




